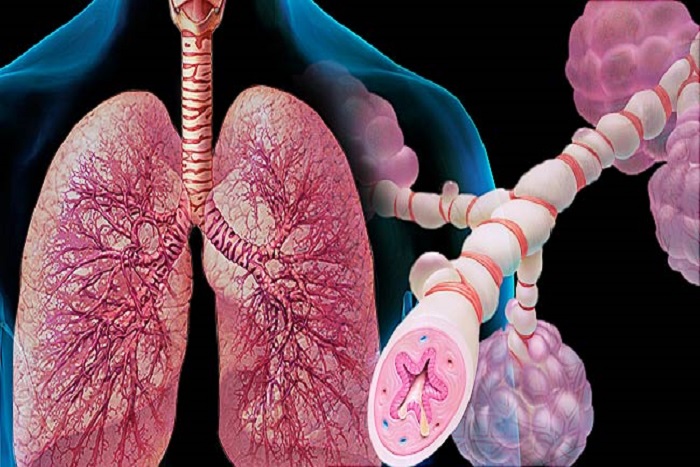
Asthma is a chronic respiratory disorder characterised by variable airway inflammation, airway obstruction, and airway hyper-responsiveness. These features interact to determine the clinical symptom pattern of the individual. While the majority of asthmatic children have an intermittent symptom phenotype, the minority have persistent symptoms, reflecting the underlying chronic inflammation. In older children, as in adults, this may lead to permanent structural alterations of the airway wall (airway remodelling) and potentially a more severe asthma phenotype.
This topic covers the treatment of children up to 12 years of age. Children 12 years and older are treated the same as adults, except for emerging therapies such as bronchial thermoplasty. Please see our Asthma in adults topic for more information.
Symptoms
Not all children have the same asthma symptoms, and these symptoms can vary from episode to episode in the same child. Possible signs and symptoms of asthma in children include:
While these are some symptoms of asthma in children, your child's doctor should evaluate any illness that complicates your child's breathing. Many pediatricians use terms like "reactive airways disease" or bronchiolitis when describing episodes of wheezing with shortness of breath or cough in infants and toddlers (even though these illnesses usually respond to asthma medications). Tests to confirm asthma may not be accurate until after age 5.
Risk factors
There are many risk factors for developing childhood asthma. These include:
Diagnose
Asthma in children can often be diagnosed based on medical history, symptoms, and a physical exam. Keep in mind that oftentimes when you take your infant or older child to the doctor with asthma symptoms, the symptoms may be gone by the time the doctor evaluates the child. That's why parents are key in helping the doctor understand the child's signs and symptoms of asthma.
Avoiding triggers, using medications, and keeping an eye on daily asthma symptoms are the ways to control asthma in children of all ages. Children with asthma should always be kept away from all sources of smoke. Proper use of medication is the basis of good asthma control.
Based on your child's history and the severity of asthma, his or her doctor will develop an Asthma Action Plan and give you a written copy. This plan describes when and how your child should use asthma drugs, what to do when asthma gets worse (falls into the yellow or red zones), and when to seek emergency care for your child. Make sure you understand this plan and ask your child's doctor any questions you may have.
Your child's written Asthma Action Plan is important to the successful control of his or her asthma. Keep it handy to remind you of your child's daily asthma management plan as well as to guide you when your child develops asthma symptoms. Also make sure your child's caregiver and school teacher has a copy of the Asthma Action Plan, so they will know how to treat the child's symptoms if she should have an asthma attack away from home.
For more information and for a printable asthma action plan, see WebMD's article on Developing an Asthma Action Plan.